10 Nursing Programs with Clinical Hour Requirements
Choosing a nursing program means looking beyond tuition and rankings. Clinical hours are where classroom learning becomes real patient care. Different program pathways set different expectations for required in-person and simulated clinical experiences. State boards of nursing and accreditors influence minimums and acceptable use of simulation, while individual schools set exact hour totals and placement policies. Some programs list explicit hour counts in handbooks; others describe competency-based requirements instead. Before you apply, know three things to verify: the program’s total required clinical hours, how many of those can be fulfilled with simulation, and whether the school assists with local clinical placements. If you’re comparing options, gather the program clinical handbook and contact the clinical placement coordinator early. That information will tell you when rotations happen, what specialties you’ll cover, and which types of preceptors supervise your shifts. This guide breaks down clinical-hour expectations across ten common nursing program types so you can compare pathways and plan your schedule, finances, and family support.
1. Associate Degree in Nursing (ADN)

ADN programs are two-year options focused on preparing students for entry-level registered nursing practice and the NCLEX-RN. A commonly cited benchmark is that ADN programs include at least 400 hours of in-person clinical experience, though exact totals vary by school and state. Those clinical hours are typically organized into rotations covering medical-surgical care, maternal-newborn, pediatrics, mental health, and community nursing. Students should expect supervised shifts at partner hospitals or clinics where an experienced RN or faculty member acts as preceptor. Simulation labs usually prepare students before they enter clinical sites, and many programs combine simulation with live patient care to build confidence and skills. If you choose an ADN, check the program’s clinical handbook for placement policies, the typical weekly hour load during clinical semesters, and whether the program helps arrange sites close to where you live. Knowing the clinical schedule in advance helps plan work, childcare, and transportation needs.
2. Traditional Bachelor of Science in Nursing (BSN)

A four-year BSN covers broader clinical content than many shorter tracks, with rotations across multiple specialties and settings. BSN curricula emphasize leadership, public health, and community practice in addition to core nursing skills. Because of that wider scope, BSN students usually accumulate more hands-on clinical experiences than ADN students. Typical clinical placements include adult medical-surgical units, pediatrics, obstetrics, psychiatric settings, and community health. Programs also arrange simulation experiences that mirror complex scenarios students might not see frequently in practice. Each program sets its own total clinical hours and scheduling cadence, so you’ll see variation between campuses and between accelerated and traditional tracks. Before enrolling, request the clinical hour breakdown, ask which rotations are mandatory, and verify whether the program’s accreditor reports list minimum competencies or hour totals. That helps you understand both how clinical learning is sequenced and what practical skills you’ll graduate with.
3. Accelerated BSN (ABSN)

Accelerated BSN tracks compress the full BSN curriculum into a shorter timeframe for students who already hold a bachelor’s degree in another field. Because the program must cover the same competencies in less time, clinical rotations are intense and scheduled back-to-back. Accelerated programs aim to provide equivalent clinical exposure to a traditional BSN, though students complete those hours in a condensed calendar. Expect full days of coursework and clinicals during clinical semesters, and plan for limited flexibility with paid work. Programs lean on simulation to prepare students quickly before patient care and to ensure consistent skill practice. If you’re considering an ABSN, ask how the school balances simulated versus in-person hours, whether clinical sites are guaranteed for all students, and what support exists for finding preceptors. That information clarifies whether the accelerated pace fits your schedule and learning style.
4. RN-to-BSN Programs

RN-to-BSN programs are designed for licensed nurses who want a bachelor’s degree and typically focus on leadership, community health, and evidence-based practice. Many RN-to-BSN tracks reduce or waive clinical hours that duplicate prior RN experience, instead requiring shorter practicums tied to population health, leadership projects, or care coordination. Some programs require a small, focused practicum—often in community settings or through a capstone experience—while others accept documented recent clinical practice in lieu of additional hours. Verify whether a program requires a specific number of supervised clinical hours, what documentation of prior practice the school accepts, and whether the practicum can be completed at your current workplace. That helps you determine how much additional hands-on time you’ll need and how quickly you can finish the BSN.
5. LPN/LVN-to-RN Bridge Programs

LPN- or LVN-to-RN bridge tracks build on practical nursing experience and focus on filling gaps needed for RN-level competencies. Clinical requirements typically include hands-on rotations that align with ADN-level expectations so learners meet entry-level RN skills. While licensed practical experience can shorten some classroom requirements, most bridge programs still require supervised clinical placements in acute care, medical-surgical, or specialty units. Programs often pair classroom modules with clinical lab practice and community placements to reinforce safe decision-making at a higher scope. If you’re coming from an LPN/LVN background, confirm which prior experiences the school will accept and whether any additional clinical hours are required beyond simulated competency demonstrations. Also ask about placement assistance and preceptor availability since scheduling can be competitive in busy clinical sites.
6. Direct-Entry/Entry-Level MSN (for non-nurses)

Direct-entry or entry-level MSN programs let people with non-nursing bachelor’s degrees earn a master’s and become licensed RNs. These pathways combine pre-licensure clinical hours needed for RN competence with graduate-level clinical experiences tied to advanced practice or specialty training. Expect substantial total hands-on time because you’re completing both foundational RN clinicals and advanced practicum components. Programs vary dramatically in how they count and sequence hours, and state boards may require documentation of pre-licensure clinical hours before testing for licensure. If you’re evaluating direct-entry MSN options, request the full clinical-hour breakdown for both the pre-licensure and graduate sections. Also check whether the school’s graduate clinicals meet certification board requirements for any advanced role the program prepares you for.
7. Master of Science in Nursing — Nurse Practitioner (MSN-NP)
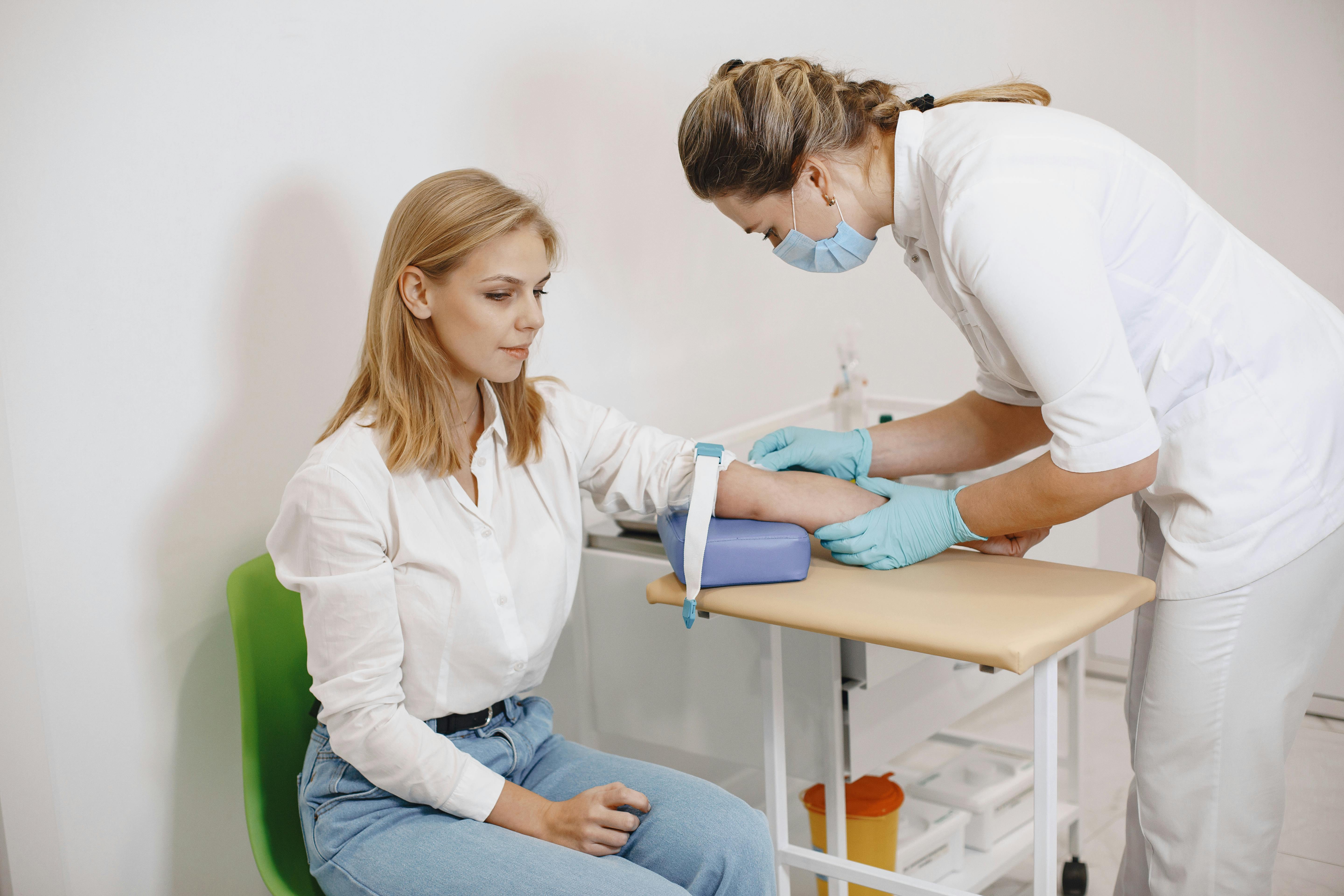
NP programs center on advanced clinical practicum hours required for national certification and state licensure as an advanced practice provider. Many NP tracks require several hundred supervised clinical hours in the chosen specialty, with placements in primary care, pediatrics, acute care, or psychiatric settings depending on the concentration. Preceptors must often meet program criteria and provide direct supervision, documentation, and evaluation. Programs differ on how they log hours, what counts as direct patient contact, and whether telehealth encounters are acceptable. Always confirm with the program which certifying body the clinical hours target, how many total supervised hours are needed for graduation, and what the school requires for preceptor qualifications and liability coverage. This prevents surprises at the point of seeking certification.
8. Doctor of Nursing Practice (DNP)
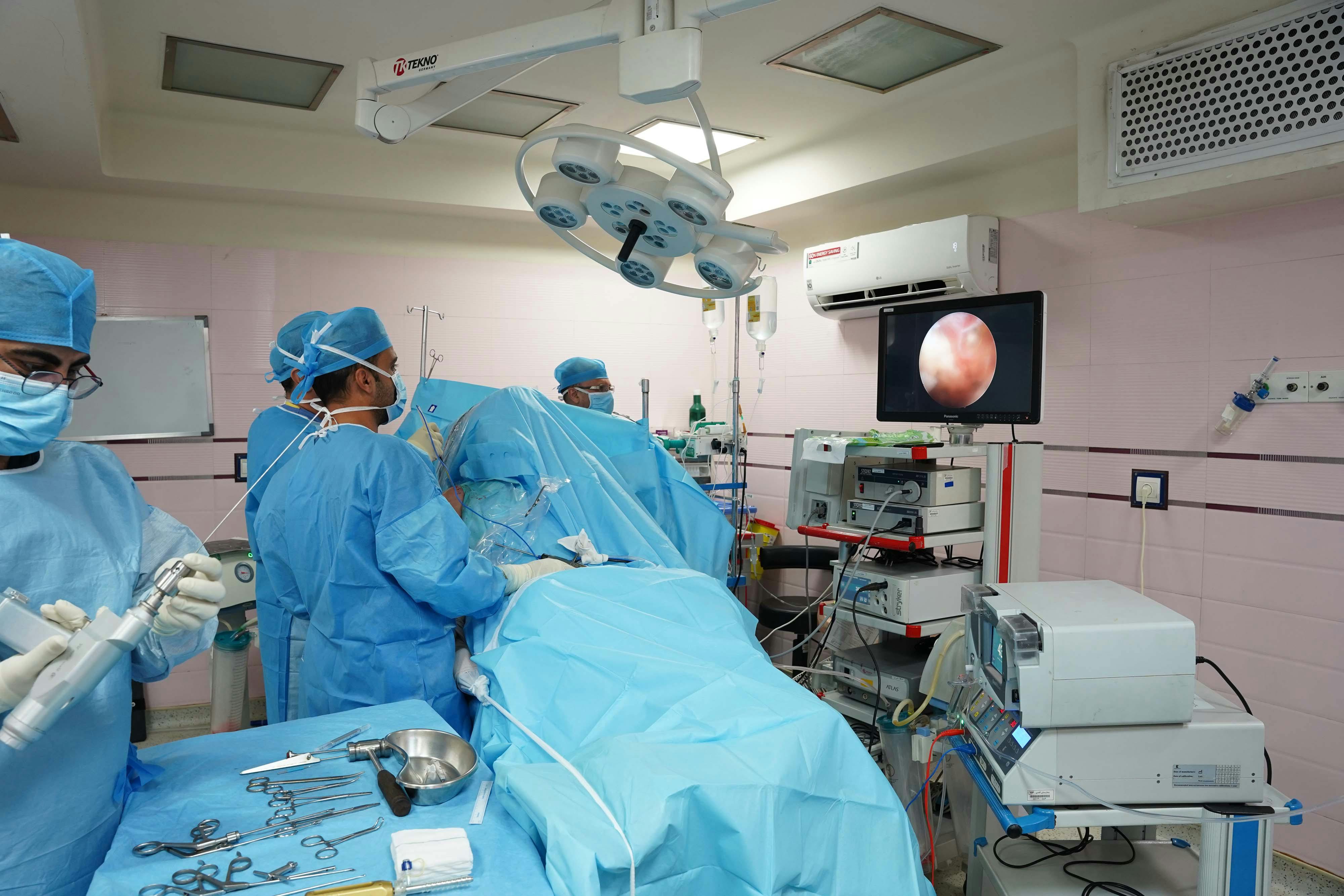
DNP programs include advanced clinical practice hours plus a practice-focused scholarly project or residency. Requirements vary by entry point: BSN-to-DNP pathways often include a significant number of post-baccalaureate practice hours, while DNPs for those who already hold advanced practice credentials may focus on specialization hours and project-related clinical time. Accreditation guidance emphasizes practice hours tied to the program’s learning outcomes, and many schools document clinical totals separately for coursework and residency components. Before applying, review whether the DNP pathway requires additional supervised practice hours beyond what you already hold, how the school documents them, and whether the clinical residency aligns with your intended practice role. That helps you estimate timeline and site commitments.
9. Online Nursing Programs with Local Clinical Placements

Online and hybrid nursing programs pair remote didactic coursework with in-person clinicals arranged at approved local sites. These programs vary in how they secure placements: some assign an on-campus clinical coordinator who sets up local preceptors, while others expect students to find approved sites in their community. If you live in a rural area, confirm that the program approves out-of-state placements and whether the school handles background checks, immunization verification, and malpractice coverage. Ask how many of the program’s clinical hours are typically completed locally, whether simulation can reduce travel, and whether weekend or evening options exist. Clear answers will help you balance remote study with reliable, in-person clinical training.
10. Simulation-Heavy Programs and Clinical Hour Substitutions

Many schools use high-fidelity simulation to replace or supplement some in-person clinical hours, especially for rare or high-risk scenarios. Accrediting agencies and state boards set limits on how much simulation may substitute for direct patient care, and policies differ by jurisdiction. Programs that rely more on simulation typically document equivalencies between simulated scenarios and clinical competencies and will list the maximum percentage of clinical hours that simulation can cover. If a program advertises extensive simulation use, ask for the program policy on simulation-to-clinical ratios, how simulated hours are assessed, and whether employers recognize simulation-heavy transcripts. That helps you judge whether the balance between simulated and live patient hours meets your learning needs and licensure expectations.
Final takeaways and next steps

Clinical hour expectations change by pathway, state, and school. Some programs state clear hour totals; others describe competency-based requirements. Start your verification by requesting the program clinical handbook and checking the state board of nursing for any minimums or simulation rules. Ask the admissions or clinical placement office specific questions: total required in-person hours, simulation allowance, how placements are assigned, and whether the program documents hours for licensure or certification boards. For graduate clinical tracks, confirm preceptor criteria, whether telehealth counts, and certification-related hour targets. Put documentation in writing when possible so you can compare offers and plan financially and logistically. With that clarity, you’ll choose a program that matches your career goals, learning style, and life commitments.